* trigger warning – birth trauma/abuse *
The concept of ‘moral injury’ in midwifery is being recognised at last. Here, we repost in full an article by Lynn Genevieve originally published in our magazine, Midwifery Matters in Summer 2019. Lynn introduces a concept related to post-traumatic stress in this analysis of the harm it causes when we are forced to collude with a system against our values.
“Please don’t,” she begs through her tears, “it hurts my hips.” My eyes sting, and I consciously adopt my wellpracticed professional face, blank, emotionless. It is a real effort, but I’ve had lots of practice now.

Following the guidelines
This was just weeks before I left hospital midwifery practice forever. A rather fortuitous course of events meant that I was able to second to a private birth centre covering a maternity leave before moving on to community midwifery in another Trust. Fortunate indeed, as if I’d stayed, it was always going to be a choice between my health and wellbeing, or my career.
What I did not know at the time, was that I was accumulating experiences that were contributing to a form of Post Traumatic Stress Disorder (PTSD) that I now realise, never really left my practice completely. Years later, as an independent midwife, every time I entered a hospital I felt the creeping fear and panic of those early experiences. By this time, though, I had really mastered the professional facade, my armour was strong.
A lot has been written about PTSD and birth, but the vast majority is from the woman’s perspective rather than the midwife’s. I’ve met a lot of traumatised midwives in my time, and most of us were woefully ignorant of our damage.
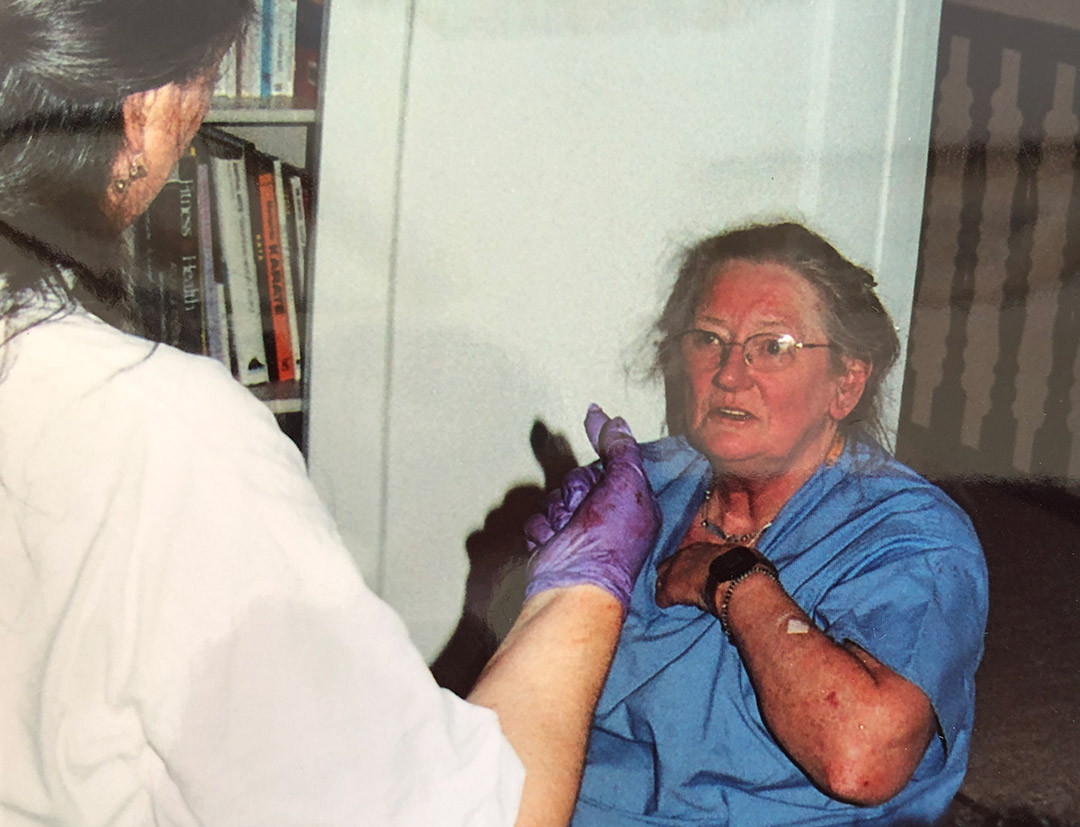
Moral Injury does not only affect soldiers
One of the problems is recognising moral injury, as the condition was pertinent in relation only to soldiers initially. When it came to health workers, the term burnout has been more often, erroneously applied. Most of us are quite familiar with burnout, and the collection of symptoms associated with it. Indeed today, I’m certain that most midwives suffer one or more of these in their work, at least some of the time such as: cynicism, decreased productivity, exhaustion.
Midwives stay in the system as they are committed. They have a ‘calling’, a vocation to be a midwife, and have come through a challenging training often involving debt, sacrifice, and guilt. I reminded myself of my own journey in researching this article by reading my ‘Diary of a Student Midwife’ which was published regularly in the early 1990’s in the NCT magazine New Generation. I’d forgotten much. It wasn’t unusual for me to drive over 100 miles to deposit children at a grandparent in the holidays before going on a shift. I described shifts ending in tears, the stress of completing a course that demanded 100% attendance in lectures and shifts; if sick, we had learning contracts to complete for theory and spent days off working to make up time. To suggest that any midwife is not ‘resilient’ is insulting, I believe.
Examinations and assault
During the preparation of this article, an excellent feature on a piece of research was published in the AIMS journal (2019, Patterson J, Vol 30, No 4). The title, ‘Traumatised Midwives; Traumatised Women’ caught my attention. The focus of the article is how women and midwives respond to PTSD and goes someway to explaining why a damaging and judgmental culture grows, as Patterson identifies that “. . . witnessing women experiencing potentially traumatic birth events may compromise midwives’ abilities to maintain positive interactions with women.” Essentially, midwives adapt their behaviour as a form of survival within the toxic environment of many NHS maternity services changing from offering a midwifery model of ‘Care as Gift’ to a medicalised model of ‘Vigil of Care’. Burnout is identified and belief in the birth process is eroded as midwives modify their actions enabling them to stay within their job, but leaves them struggling for any satisfaction in their role. This is where the word resilience becomes fashionable. It is bandied around like a badge of honour, that only worthwhile midwives earn, the ones not breaking down. This is at best, unfair, at worst, bullying. What is starting to be realised is that burnout in itself, is a symptom of an increasingly broken healthcare system and Patterson is clear where the responsibility lies.
What I found particularly interesting is that what Patterson discusses, includes an element of Moral Injury, I believe, although it is not specified. The nearest was a ‘Take home point’ that “ . . . conflict between models of midwifery care and working within toxic culture . . .” can lead to Secondary Traumatic Stress (STS). I was left wondering if Moral Injury appears in her PhD research at all? STS is what Patterson identifies midwives experiencing, a normal response to witnessing trauma. I have concluded that the difference between STS and Moral Injury is the resistance to modifying behaviour from a midwifery model to a medicalised model, either intentionally or by virtue of inability to change. And thank goodness for that, as to ‘give in’ or adapt, according to Patterson means midwives, “ . . . may suppress their emotions and present a hardened demeanour . . .” , so I am thankful that I did not ‘only’ experience STS. The silver lining though, is perhaps that women and midwives may not be suffering in vain and that by not conforming, by actually leaving the profession an important issue can be acknowledged. Perhaps there is hope that as more research is published, a change in the culture of the NHS can be embraced.
From Moral Injury to autonomy
References
- Hall, Jenny (2003) ‘Examinations and Assault – what is going on?’ in The Practising Midwife, 6 (7) p. 4
- Patterson, Jenny (2019) ‘Traumatised Midwives, Traumatised Women’ in AIMS Journal, 30 (4) https://www.aims. org.uk/journal/item/traumatisedmidwives-traumatised-women
First published in Midwifery Matters 161 Summer 2019


This was such an excellent blog and one I identified with completely. I feel now I have a name for something’s I experience every day. Thank you for writing it.
As a newly qualified midwife questioning frequently if I lack the “resilience” required to remain in the profession and oft feeling inadequate for my doubts that plague me, this article is like a healing balm, I now wonder if those who aren’t questioning or doubting are in a worse position.
Thankyou so much for writing it and sharing it.
Thanks so much for this very valuable reflection and blog. I must admit to not coming cross the term Moral Injury until after completing my PhD research and writing this article. However, it is absolutely spot on. I did come across the call for PTSD to be renamed PTSI (post traumatic stress injury). The use of the word injury is critical because it reflects what happened to someone, rather than a sense of disorder or indeed lack of resilience. I totally agree midwives are hugely resilient, in many ways this is essential so that midwives can engage with the challenging and distressing birth outcomes/procedures that can occur. BUT!! no midwife should need to develop resilience to a damaging culture – this is where we need to draw the line in expecting midwives to develop resilience. I am involved in some other work now where Moral Injury for midwives and maternity professionals is at the heart of what we are looking at. thanks Genevieve.
I was very pleased to hear that you are following up your work in such a valuable area, Jenny. Yes – the word injury is vital to understanding this area more fully. I look forward to to hearing more about this in the future with hopefully, action that affects positive change. I appreciated your comments thank you.
Jenny! Hi, I would love to talk to you about your current work. I am currently working on something similar, supporting midwives to name what they are experiencing. My NHS email is k.greenstock@nhs.net. Look forward to hearing from you!
Thank you so much for this reflection and blog. I too can relate and identify with this. Thank you so much Lynn Genevieve